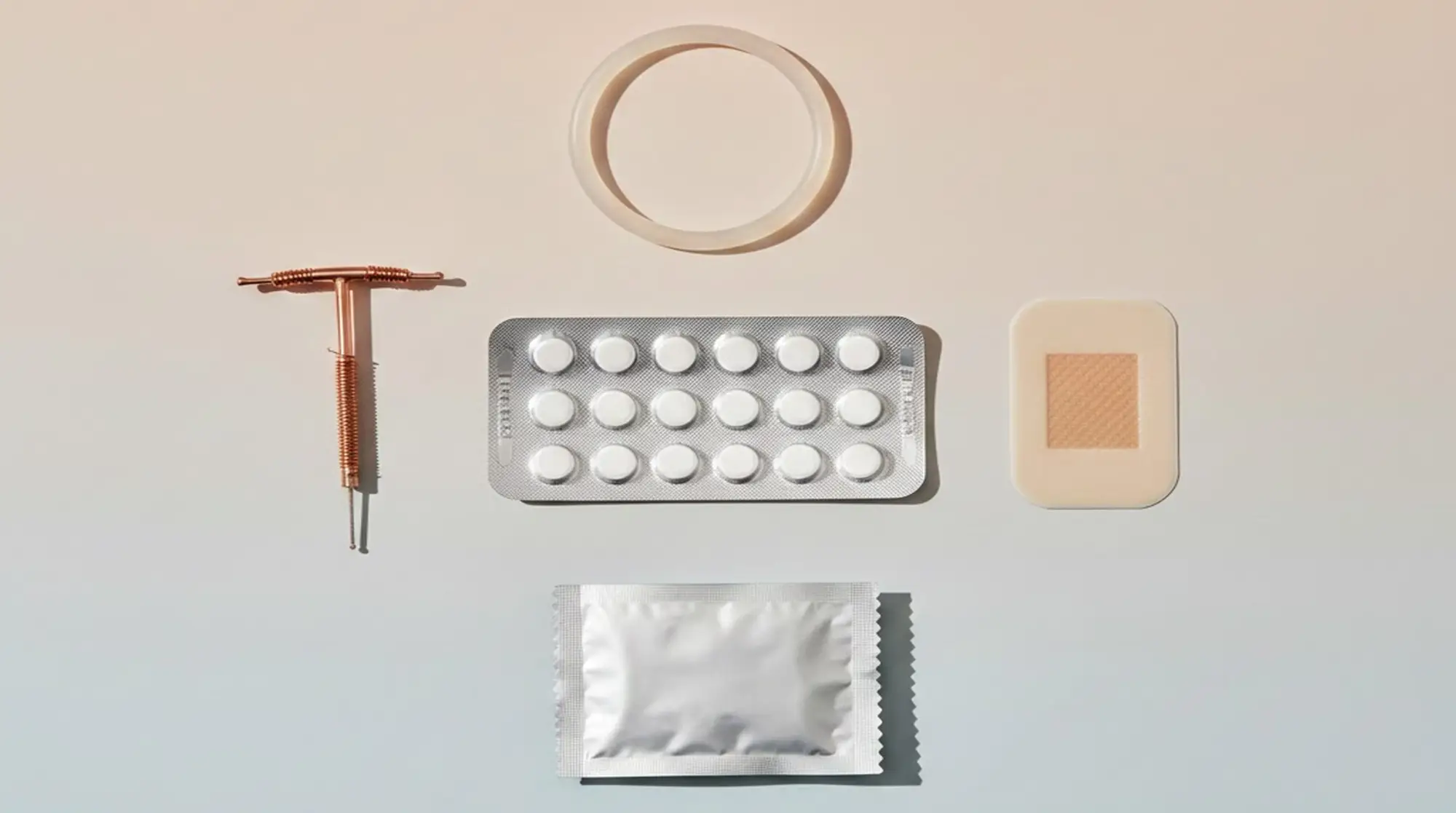
A Side-by-Side Comparison of Every Option
Your evidence-based guide to finding the best birth control method for your body, lifestyle, and plans
If you are searching for the best birth control method, you are not alone. Many Filipinos want something effective, safe, affordable, and easy to fit into real life. The truth is: there is no single “best” contraceptive for everyone. The best birth control in the Philippines is the one that matches your health needs, comfort level, budget, and future fertility plans.
This definitive guide gives you a clear, side-by-side birth control comparison (Philippines) covering the most common options available locally. It is built on the latest guidance from the World Health Organization (WHO), the Philippine Department of Health (DOH), and major sexual and reproductive health bodies.
You will find:
- A Featured Snippet-ready answer to “best birth control method”
- A detailed comparison table (typical vs perfect use, cost, side effects, convenience, reversibility)
- Filipino-specific tips on where to get each method
- A quick RH Law note on your right to family planning information and services
Quick Featured Snippet Answer
What is the best birth control method in the Philippines?
The best birth control method depends on your situation. In general, long-acting reversible contraceptives (LARCs) like implants and IUDs are the most effective for typical use because they remove daily or monthly user error. Pills, injectables, condoms, fertility awareness, and permanent methods are also valid options depending on your health, preferences, and whether you want children later. Talk to a licensed OB-GYN or trained health provider to choose safely and confidently.
How to Use This Guide
To keep things practical, this guide compares methods using criteria that most people care about:
- Typical vs Perfect Use Efficacy
- Typical use = real life with occasional mistakes
- Perfect use = consistent, correct use every time
- Cost (Estimated Local Range)
- Prices vary by brand, clinic, city, and whether you use public services
- Many methods are free in DOH and PhilHealth-supported facilities
- Side Effects
- What you might feel or notice
- Duration and Convenience
- How long it lasts and how much effort it needs
- Reversibility and Return to Fertility
- How quickly fertility returns after stopping
Side-by-Side Comparison Table (Philippines)
Note: Efficacy rates are global evidence summaries used by WHO-aligned programs. Costs are approximate Philippine ranges based on pharmacy and clinic pricing, plus DOH and PhilHealth announcements. Public facilities may offer methods free or subsidized.
| Method | Typical Use Efficacy | Perfect Use Efficacy | Estimated Local Cost | Common Side Effects | Duration / Convenience | Reversibility / Return to Fertility |
|---|---|---|---|---|---|---|
| COCs (Combined Oral Contraceptives) | ~93% | >99% | ₱150–₱900 per month (varies by brand); often free at health centers | Nausea, breast tenderness, spotting, mood changes; rare clot risk in some users | Daily pill, same time every day | Fully reversible. Fertility usually returns quickly after stopping |
| POPs (Progestin-Only Pills) | ~93% | >99% | ₱200–₱1,000 per month; can be free in public clinics | Irregular bleeding, headaches, breast tenderness | Daily pill, stricter timing than COCs | Fully reversible. Fertility returns quickly |
| Copper IUD | >99% | >99% | Private clinics often ₱10,000–₱15,000 all-in; free or PhilHealth-covered in public facilities | Heavier/longer periods early on, stronger cramps | Works up to 10+ years, no daily action | Fully reversible. Fertility returns immediately after removal |
| Hormonal IUD (LNG-IUD) | >99% | >99% | Higher private cost (often ₱18,000+); may be free in select public/PhilHealth sites | Lighter periods or no periods, spotting early | Works ~3–8 years depending on type | Fully reversible. Fertility returns quickly after removal |
| Implants (Subdermal) | >99% | >99% | ₱5,000–₱15,000 private; PhilHealth and DOH sites may offer free | Irregular bleeding, weight change, acne, mood shifts | Works 3–5 years, “set and forget” | Fully reversible. Fertility returns quickly after removal |
| Injectables (3-month shots) | ~96% | >99% | ₱120–₱400 per shot in pharmacies; free in many public clinics | Irregular bleeding, weight gain, delayed fertility return in some | Every 3 months, must be on schedule | Reversible. Fertility may take months to return after last shot |
| Condoms (Barrier Methods) | ~87% | ~98% | ₱20–₱300+ per pack; free in barangay health centers | Latex allergy in some, irritation if dry or wrong fit | Use every sex act, also STI protection | Immediately reversible, fertility unaffected |
| Fertility Awareness Methods (FAM) | ~76–88% | ~95–99% | Low or none; may buy thermometer/apps | No medical side effects, but requires discipline | Daily tracking, abstinence or backup on fertile days | Immediately reversible, fertility unaffected |
| Permanent Methods (BTL, Vasectomy) | >99% | >99% | Often free in public hospitals via PhilHealth; private fees vary | Surgical risks, short recovery | One-time procedure | Intended permanent. Reversal is difficult and not guaranteed |
Method-by-Method Breakdown
1. Combined Oral Contraceptives (COCs)
What they are: Pills containing estrogen and progestin. They prevent ovulation and thicken cervical mucus. WHO and DOH consider them safe for most healthy non-smokers without certain medical risks.
Pros:
- Regulates periods and can reduce cramps or acne
- Easy to stop anytime
- Widely available in drugstores
Cons:
- Must be taken daily
- Some users cannot take estrogen (for example, certain migraine, clot risk, uncontrolled hypertension)
Cost and access in the Philippines:
- Commonly ₱150–₱900/month depending on brand and pharmacy.
- Free in many barangay health centers and city health offices under the national FP program.
Action step:
Talk to your doctor if you have migraine with aura, high blood pressure, or smoke regularly, because these can change what is safest for you.
2. Progestin-Only Pills (POPs)
What they are: Estrogen-free pills, often recommended for breastfeeding people or those who cannot take estrogen.
Pros:
- Safe for more medical conditions than COCs
- Good option postpartum or during breastfeeding
Cons:
- Timing matters more. Late pills reduce effectiveness
- Irregular spotting is common early on
Cost and access:
- Similar to COCs, often ₱200–₱1,000/month depending on brand.
- Available in public clinics and some DOH facilities.
Action step:
If you want a pill but hate hormone swings from estrogen, ask your OB about POPs.
3. Intrauterine Devices (IUDs)
Copper IUD
What it is: Non-hormonal device placed in the uterus. Prevents fertilization and can last 10 years or more.
Pros:
- Highest real-life effectiveness
- No daily or monthly work
- Hormone-free
Cons:
- Periods may be heavier or crampier in the first months
Cost and access:
- Private placement is often ₱10,000–₱15,000 all-in.
- DOH and PhilHealth-supported public hospitals offer IUDs free or fully covered.
Action step:
If you want a long-term method without hormones, ask about copper IUD suitability.
Hormonal IUD (LNG-IUD)
What it is: Releases low-dose progestin locally, often reduces bleeding and cramps.
Pros:
- Very effective
- Many users get lighter periods or none at all
Cons:
- Spotting for the first months is common
- Higher private cost
Access:
- Available in some private clinics and select public programs, depending on local supply.
Action step:
If your periods are heavy or painful, a hormonal IUD may double as symptom relief. Ask your provider.
4. Implants (Subdermal)
What they are: Thin rods inserted under the skin of the upper arm, releasing progestin for 3–5 years.
Pros:
- One of the most effective methods in typical use
- Works for years with no daily effort
- Safe for many users who cannot take estrogen
Cons:
- Unpredictable bleeding patterns are common early on
- Requires trained provider for insertion and removal
Cost and access:
- Private clinics: roughly ₱5,000–₱15,000 depending on facility.
- Public hospitals and health centers may provide implants free through PhilHealth or DOH programs.
Action step:
If you want “set and forget” protection and do not mind a small procedure, this is a top option to discuss.
5. Injectables
What they are: Progestin shots given on a schedule, typically lasting about 3 months per injection.
Pros:
- Private and discreet
- No daily pill
- Helpful for users who forget pills
Cons:
- Must return on schedule
- Some users experience weight change or irregular bleeding
- Fertility return may be delayed after stopping
Cost and access:
- Pharmacy prices can start around ₱120–₱400 per shot depending on brand and location.
- Injectables are commonly free at barangay and city health centers.
Action step:
If you may want pregnancy soon after stopping, tell your doctor, because shot users sometimes need extra time for fertility to return.
6. Condoms and Other Barrier Methods
What they are: Physical barriers that prevent sperm from entering the uterus. Condoms are the most common barrier method in the Philippines.
Pros:
- Only method here that protects against STIs
- Easy to buy and use
- No hormones
Cons:
- Effectiveness depends on correct use every time
- Can break or slip if wrong size or technique
Cost and access:
- Drugstores, convenience stores, online shops
- Often free in barangay health centers, especially for young adults and public health programs.
Action step:
Even if you use another method, condoms are smart for new or multiple partners for STI protection.
7. Fertility Awareness Methods (FAM)
What they are: Natural methods that rely on tracking fertility signs to avoid sex or use backup on fertile days. WHO and DOH recognize these as valid methods when taught and used correctly.
Pros:
- No hormones or devices
- Low cost
- Works for people who want a natural approach
Cons:
- Requires daily tracking and strong discipline
- Typical use effectiveness is lower due to real-life variability
Cost and access:
- Can be taught in some public clinics and NGOs
- Tools like tracking apps or thermometers may add small costs
Action step:
If you want FAM, ask for a trained counselor and consider using condoms during learning months.
8. Permanent Methods (BTL and Vasectomy)
What they are: One-time procedures intended to permanently prevent pregnancy.
Pros:
- Highest effectiveness
- No ongoing cost or maintenance
Cons:
- Intended permanent, reversal is difficult and not guaranteed
- Requires medical procedure
Cost and access:
- Free in many public hospitals through PhilHealth and DOH family planning packages.
- Available privately with varying fees.
Action step:
If you are sure you do not want future pregnancies, discuss permanent options with your partner and provider.
Where to Get Birth Control in the Philippines (Accessibility and Availability)
Thanks to the DOH Family Planning Program and Universal Health Care efforts, most methods are legally available and widely distributed.
Public Options (often free):
- Barangay Health Centers
- City or Municipal Health Offices
- DOH-retained hospitals
- PhilHealth-accredited FP clinics under “Tamang Sagot”
Private Options:
- OB-GYN clinics
- Hospitals
- Women’s health NGOs
- Licensed pharmacies (Watsons, Mercury Drug, Southstar Drug, etc.)
Tip for Filipino users:
If cost is a concern, start with your barangay health center. You can ask what is currently in stock or if there is a schedule for implants, IUD insertion, or counseling days.
The RH Law Context: Your Rights Matter
The Responsible Parenthood and Reproductive Health Act of 2012 (RA 10354) guarantees Filipinos the right to:
- Accurate, unbiased family planning information
- Access to medically safe and effective contraceptive methods
- Prioritization of free methods for the poor and marginalized
In simple terms: you have a legal right to know your options and access them safely, whether you choose modern or natural methods.
How to Choose the Best Birth Control Method for You
Ask yourself these five questions:
- How important is “no daily effort”?
If you want the least maintenance, consider IUDs or implants. - Do you want kids later? When?
Most methods are reversible. If you want pregnancy soon after stopping, pills, condoms, IUDs, implants, or FAM may be easier than injectables. - Do you need STI protection?
If yes, use condoms, even with another method. - How do you feel about hormones?
If you want to avoid hormones, look at copper IUD, condoms, or FAM. - What is your realistic budget?
Use public services if you want zero cost or subsidized care.
Best practice: talk with a licensed provider. The DOH handbook emphasizes informed choice and client-centered counseling as the standard of care in the Philippines.
Safety Notes and Disclaimers
This guide is for education only. It does not replace medical advice.
Only a licensed health professional can:
- Confirm what is safe for your medical history
- Screen for contraindications
- Provide correct use guidance
If you have conditions like hypertension, migraines, clotting issues, diabetes, smoking history, or you are postpartum or breastfeeding, do not self-select a method without medical input.
The “best birth control method Philippines” is not a universal winner. It is the method that you can use consistently, safely, and confidently.
- If you want maximum effectiveness with minimal effort, implants and IUDs are top options.
- If you want control without procedures, pills or injectables may fit.
- If you need STI protection, condoms are essential.
- If you prefer hormone-free living, explore copper IUD, condoms, or fertility awareness.
- If your family is complete, permanent methods may be right.
Next step:
Book a consultation at your barangay health center or OB-GYN clinic and say:
“I want help choosing the method that fits my body and plans. Can we go through my options together?”
You deserve care that is informed, respectful, and built around your life.
Leave a Reply